
Welcome to Derm Diaries, where we delve into dermatological conditions we frequently encounter in our practice. Today, we’re shedding light on a condition that has become increasingly prevalent in recent years: Frontal Fibrosing Alopecia (FFA). If you or someone you know is experiencing hair loss along the hairline, sideburns, or eyebrows, accompanied by small, flesh-colored bumps on the face, this article is for you.
What is Frontal Fibrosing Alopecia?
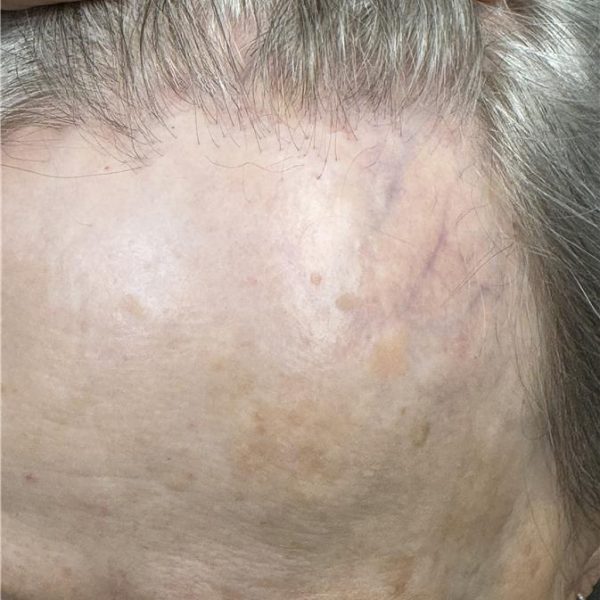
Frontal Fibrosing Alopecia is a type of scarring hair loss that primarily affects the frontal scalp line. It is characterized by a receding hairline, often progressing slowly over time. This condition can also involve hair loss from the sideburns and eyebrows, and some patients may notice small, flesh-colored bumps on the face, which are perifollicular papules—a hallmark feature of FFA.
Etiology: What Causes FFA?
The exact cause of FFA remains unclear, but research suggests a combination of genetic predisposition and environmental triggers. Some potential contributing factors include:
• Hormonal influences: The condition predominantly affects postmenopausal women, indicating a possible link to hormonal changes.
• Immune dysregulation: FFA is considered an autoimmune condition where the body mistakenly attacks its own hair follicles.
• Environmental exposures: Emerging studies point to possible links with certain skincare products, sunscreens, or other topical agents.
Pathogenesis: How Does FFA Develop?
Under the microscope, FFA shows features consistent with lichen planopilaris, its closest related condition. The following inflammatory changes are observed:
1. Perifollicular inflammation: Lymphocytes cluster around hair follicles, leading to follicular destruction.
2. Fibrosis: Over time, the inflammation triggers scarring (fibrosis), replacing the hair follicle with connective tissue.
3. Sebaceous gland loss: The glands associated with hair follicles are often destroyed early in the disease process.
This inflammatory and fibrotic process results in irreversible hair loss, emphasizing the importance of early diagnosis and intervention.
Clinical Presentation
Patients with FFA often present with:
• A progressively receding frontal hairline
• Loss of eyebrow hair
• Hair loss extending to the sideburns
• Flesh-colored perifollicular papules on the face
• Occasionally, mild redness or itching in the affected areas
Treatment Options
While there is no cure for FFA, early intervention can help halt progression and preserve remaining hair. Treatment focuses on reducing inflammation and modulating the immune response. Options include:
Topical Treatments
• Topical corticosteroids: To reduce inflammation at the scalp.
• Calcineurin inhibitors: Such as tacrolimus, to suppress the local immune response.
Oral Medications
• 5-alpha reductase inhibitors: Finasteride or dutasteride to address hormonal influences.
• Hydroxychloroquine: An anti-inflammatory medication commonly used in autoimmune conditions.
• Tetracycline antibiotics: To reduce inflammation and suppress immune activity.
• Low-dose naltrexone (LDN): For its potential role in immune modulation.
Procedural Options
• Intralesional corticosteroids: Targeted injections to areas of active inflammation.
• Hair transplant surgery: May be considered in stabilized cases, although results can vary due to scarring.
Adjunctive Measures
• Minimizing environmental triggers: Avoiding potential irritants like certain sunscreens or hair products.
• Photoprotection: Sunscreen use to prevent additional damage.
• Lifestyle modifications: Stress reduction and a healthy diet may support overall skin and hair health.
The Importance of Early Diagnosis
FFA is a chronic, progressive condition, and early diagnosis is crucial to managing its effects. If you’re noticing any symptoms resembling FFA, schedule an appointment with a board-certified dermatologist. Together, we can develop a personalized treatment plan to slow the progression and preserve your hairline.
At Dermatology Solutions, we’re here to support you every step of the way. Stay tuned for more insights and updates in our Derm Diaries series!
Disclaimer: The photos shown are actual images of our patient, shared with explicit written consent. These images are for educational use only and may not be copied, distributed, or reproduced without permission from our office.