
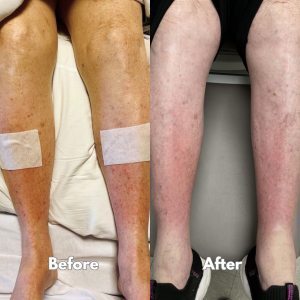
An 80-year-old woman was admitted through the ER for tight, swollen, itchy, and painful lower legs. She had been treated multiple times for “recurrent cellulitis,” with little long-term improvement. This time, her symptoms had worsened over several weeks, prompting hospitalization for evaluation and IV antibiotics.
Her medical history included hypertension, chronic stasis dermatitis, hypothyroidism, diabetes, coronary artery disease, and hypercholesterolemia—all conditions that increase the risk of vascular complications.
Dermatology was consulted to evaluate the patient during her inpatient stay and we diagnosed her with lipodermatosclerosis (LDS), a condition often mistaken for infection but requiring an entirely different approach.
After implementing appropriate treatment—focused on topical anti-inflammatories, leg elevation, compression therapy, and skin barrier repair—the patient’s pain, swelling, and skin tightness improved significantly within weeks. Her itching resolved, mobility improved, and the chronic discoloration and inflammation began to fade.
Included below are before-and-after photographs documenting her progress and the visible improvement in skin texture and color after treatment was initiated.
Lipodermatosclerosis is a chronic inflammatory condition affecting the lower legs, caused by long-standing venous hypertension and insufficiency. It presents with pain, tightness, fibrotic skin changes, and often hyperpigmentation, particularly in the lower medial calves. It is frequently misdiagnosed as cellulitis, leading to unnecessary antibiotic use.
Patients with LDS may experience:
• Progressive leg tightness or stiffness
• Swelling and pain
• Itchy, reddish-brown discoloration of the lower legs
• Indurated (hardened), bound-down skin
• Worsening stasis dermatitis
• In severe cases, ulceration or non-healing wounds
This patient had several risk factors contributing to lipodermatosclerosis:
• Chronic venous insufficiency and stasis dermatitis
• Hypertension
• Coronary artery disease
• Type 2 diabetes mellitus
• Hypercholesterolemia
• Hypothyroidism, which can contribute to delayed healing and tissue swelling
• Age over 75, which increases the risk of vascular insufficiency and chronic inflammation
The inflamed, red, swollen appearance of LDS closely mimics cellulitis, but key differences include:
• Bilateral involvement (cellulitis is often unilateral)
• Lack of systemic symptoms like fever or leukocytosis
• Chronicity or recurrence despite antibiotics
• Presence of underlying venous stasis or fibrosis
LDS stems from longstanding venous hypertension, where damaged valves allow blood to pool in the lower legs. This leads to:
• Leakage of red blood cells and fibrin into surrounding tissue
• Chronic inflammation and fibrosis of the skin and fat layer (panniculitis)
• Skin thickening, discoloration, and ulcer risk due to poor circulation
Successful management of LDS focuses on improving venous return, reducing inflammation, and preventing ulceration.
• Graduated compression stockings
• Leg elevation and ambulation
• Topical corticosteroids to calm inflammation
• Moisturizers and barrier creams for stasis dermatitis
• Pentoxifylline to enhance blood flow and reduce inflammation
• Avoidance of unnecessary antibiotics
• Endovenous laser ablation or sclerotherapy for underlying varicosities
• Skin grafting or wound care specialist referral if ulcers develop
• LDS is part of the chronic venous disease spectrum, which includes varicose veins, stasis dermatitis, and venous ulcers
• LDS can cause the “inverted champagne bottle” appearance of the legs due to skin tightening above the ankles, as seen in this patient
• Studies show up to 30% of cases diagnosed as cellulitis in older adults are actually non-infectious conditions like lipodermatosclerosis or venous stasis dermatitis
Not all red, swollen legs are infections. Lipodermatosclerosis is a chronic skin and vascular condition that requires long-term management—not just a short course of antibiotics. Accurate diagnosis is crucial to prevent unnecessary hospitalizations and improve quality of life.
Disclaimer: This case features an actual patient of Dermatology Solutions, shared for educational purposes with written patient consent. All patient images and content are protected under copyright. Reproduction, copying, or distribution without explicit written consent from Dermatology Solutions is strictly prohibited.